The Birth of Matilda
- MotherMoon

- May 25, 2021
- 10 min read
If you would like to read about the lead up to my birth head to my blog Pursuit of Felicity for my Preeclampsia Journey.

After what felt like the longest week of my life trying to induce labour at home before my scheduled induction date, Saturday rolled around and in I went. We arrived at the hospital at around 2pm and I was given a vaginal exam by a midwife who informed me that I had a bishop score of 5 and that I wouldn't need any cervical ripening methods prior to having my waters broken. All we had to do was wait until a bed in the birth suite opened up. As the hours passed by, David and I were chatting with our hypnobirthing instructor, Jess (@mothermoon_hypnobirthing), who told us a bishop score of 5 is not ideal for being induced and that it should really be an 8 or above to optimally have an ARM. She encouraged us to discuss our options with the staff using our B.R.A.I.N.S technique. The more we discussed this, the more we felt uncomfortable going ahead with the induction without cervical ripening, so by the time they wheeled me down to the birth suite at 11pm that night we had decided to advocate for ourselves and asked the obstetrician on duty for a second opinion. The obstetrician conducted a second vaginal exam (as she needed to do this anyway if we decided to go ahead and break my waters) and she actually agreed that I wasn't ready and could do with some cervical ripening. I opted to go with the cooks catheter ripening method (which Jess had taught us about), as this has less side effects than the gel. The obstetrician inserted the catheter there and then, which was essentially two small balloons, one which sat inside my uterus and one which sat in my vagina, and pumped them up with water. I was told this would be kept in for up to twelve hours, but that it may fall out beforehand. This was inserted at 11.30pm, and my gosh, what an uncomfortable feeling! It instantly brought on really intense cramping and my blood pressure shot up to 165/100, so they gave me extra blood pressure medication on top of what I was already taking for the preeclampsia, pain killers and a sleeping tablet to get through the night.
It was at exactly 11.30am the next morning (right on the 12 hour mark) that I went to the bathroom and the catheter fell out on its own. I alerted the midwife on duty who informed the birth suite that I was ready to go. Unfortunately, it wasn't until 27 hours later that a spot in the birth suite opened up as so many spontaneous births were taking place that were considered a higher priority. This meant another night in hospital (fortunately the vegan meal options were fairly decent at the RBWH) and not being taken down to birth suite until 2.30pm on Monday.
Funny story - it was at the time I was being wheeled down to birth suite that David had gone to buy me a new phone as the charger port on my existing phone had stopped working that afternoon. Luckily I had to sit in my birth suite room for another three hours until my waters were broken. During this time my first midwife for the evening helped me to set up my birth space the way I wanted as encouraged through my hypnobirthing course. For me this meant low lighting, familiar sounds (I'd set episodes of 'Friends' up on the iPad), bouncing on the birth ball, and keeping myself well fed and hydrated. At 5.30pm my waters were broken, at which point I was told my bishop score was still a 5. They basically said that as so much time had passed since the catheter had fallen out that any good work the catheter had done was no longer evident. Either way, I had been in hospital for more than 50 hours at this point, and as I was still considered a high risk pregnancy due to my preeclampsia, we needed to get things going.
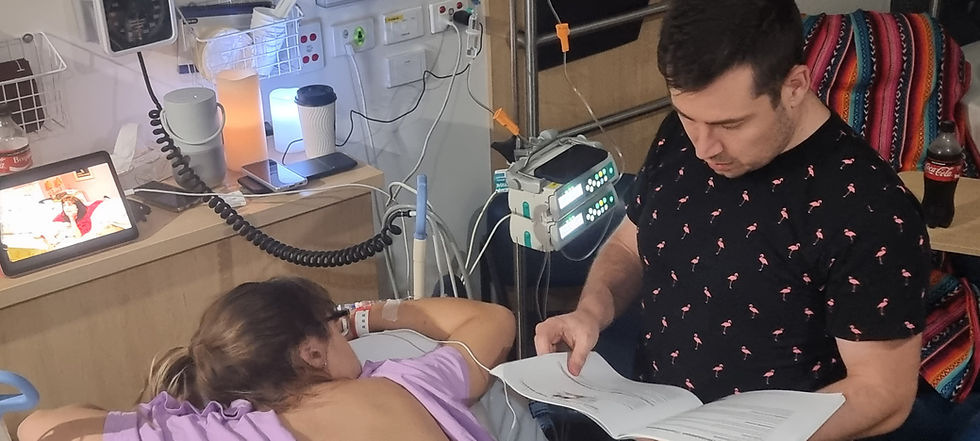
The feeling of having my waters broken wasn't that bad. The insertion of the cooks catheter was much more uncomfortable by comparison. It wasn't like the movies with a big gush of water. My recent ultrasound had shown that I had very little amniotic fluid, and as bubs head was engaged, it made sense that I would only notice a small trickle if anything. At the same time as having my waters broken, we also had a monitor inserted into bubs scalp. There is probably a more technical term for this [foetal scalp electrode or FSE], but as I will never do this again, I have no intention of remembering what it was called. Basically I was told that it would be the best way to monitor bubs heart rate during labour and would allow me to move around more freely, however it was totally unreliable and seemed to cause more issues than it did lessen them. The thought of having a monitor inserted into my child's scalp (no matter how much they claim it doesn't hurt them) still doesn't sit well with me to this day. I just keep reminding myself that preeclampsia is a serious condition that was putting my child's life at risk, and I did what we felt was best with the information we'd been given at the time. I almost wasn't going to share that we did this as I still feel so much guilt, but I think it's important to let others know that this isn't necessarily a helpful option of monitoring.
Two hours (and a few episodes of Friends later) after having my waters broken, I was hooked up to and started on the synthetic oxytocin drip. This was to bring on contractions as neither the cooks catheter or breaking of my waters had done so. The amount of synthetic oxytocin being released into my system was raised little by little every 30 minutes, and it wasn't until 9pm when my second midwife took over that I started to feel much at all. I knew early in the night that the way I would feel most comfortable contracting was on the bed, on all fours, leaning over the back of the bed. David was an amazing birth partner and set up the iPad in front of me, massaging me and advocating as needed. Prior to active labour, which kicked in around midnight, I was using a very low level of gas and air, watching Friends, and using our TENS machine on low on my lower back to mimic the feeling of being in the shower. The TENS machine and gas and air were used in time with my contractions, and I quickly adopted a rhythm and routine that made the time fly by and made the whole experience manageable. I say manageable, because let's face it, induced contractions are intense. I was under no misconception about this going into things, which is why I set myself up with the tools I needed to get through it all. I cannot thank Jess enough for all of the invaluable information, tools and support she provided us.

At midnight, going into the early hours of Tuesday (at 39+5 weeks gestation), I was given another quick vaginal exam where I learned later on that I was now 4 centimetres dilated. At the time I didn't find out how far along I was as I stated in my birth preferences that I did not want to hear numbers, as I did not want to feel disappointed and potentially halt my labour if I considered the number too low. I was, however, informed that I was now in active labour, which was really exciting and equally terrifying as I could definitely feel the contractions ramping up. It was at this point that David muted the iPad for me (but we kept Friends playing so that I had a familiar and comforting visual directly in front of me to zone out to) and used our portable speaker to play affirmations. These affirmations were super calming and helped me to focus more on my breathing. I stayed in the same position, gradually increasing the gas and air and the level on the TENS machine to match the intensity of my contractions, and focused with everything inside of me on just keeping to the routine that had been working for me so far. I know each person and labour is different, and for me in that moment, this was what worked for me. I did not want to go in the shower (despite wanting this so badly my whole pregnancy), I did not want to walk around, I simply wanted to kneel against the back of the bed frame and let gravity do its work.

At what I believe was around 2.30am, the contractions were getting super intense and I began to question whether I could continue without an epidural. My midwife prompted me to get out of bed and go to the toilet, saying that if I didn't do a wee that she would need to insert a catheter. I was so annoyed that I was having to get up and walk around, and the contractions were so intense by this point that I could barely see in front of me, but I'm pretty sure that getting up for five minutes was what brought me to the point of transition. If you don't know what transition is, it's around the last 5-10 minutes of active labour before bub is born. It's when most women truly begin to question themselves and whether they can keep going. This was the case for me, but I also knew that when I started to feel that way is when my baby would soon be here, so I was able to find comfort in this knowledge. For me, the last 10 minutes consisted of being told to lie down on my back to check my progress (and David being shown bubs head so that he could let me know that it was 'go time'), me fighting to get back on all fours as lying on my back was excruciating, and then being asked to get back on my back again as they were worried about my baby's heart rate and wanted my legs up in stirrups so that they could place external monitors onto bubs head (again, I will never do the scalp monitoring again as it was useless in the end anyway).
I wouldn't say that my birth was traumatic, but the last few minutes were very hard for me. Knowing that I would be giving birth on my back was incredibly disappointing. It was uncomfortable (I did not have gravity to help me anymore) and it put bubs head into a position where it was very painful and difficult to birth. As bubs heart rate had dipped (something I later learned is completely normal), a bunch of hospital staff ran in at the last minute, turning on all the bright lighting and talking about using a vacuum and performing an episiotomy. I was pretty much unable to advocate for myself at this point. All I could see was white, and I really had to focus in order to see the obstetrician who was now in front of me. Luckily David was well aware of my preferences and told them I wanted to tear rather than have an episiotomy. It was at this point I yelled out that I would only agree to an episiotomy if they truly believed I was at risk of a third or fourth degree tear. They could not say they believed that (how were they to know really) and instead tried to push the idea of using the vacuum, convincing us that it was needed to get bub out quickly and safely, and suggesting that I was putting bub at risk by deliberating any longer. We reluctantly agreed, overwhelmed in the moment, however the vacuum would not attach (something I am grateful for in hindsight). They again pushed for an episiotomy, and David asked that I be given a chance to push first. I pushed four times from memory, trying to visualise doing a large bowel movement (as I learned from hypnobirthing) but due to being on my back I just couldn't get bubs head out on my own. I could actually feel that bubs head was stuck, and with each push it felt like I was going to split in two. They pushed for an episiotomy once more and this time I agreed. I was in so much pain that I felt like I was going to die (I won't sugarcoat it), and hearing that bubs heart rate was dipping had me scared for his or her wellbeing. Once the episiotomy cut was made (a 1cm diagonal cut), bub was delivered with the next push at 3:11 am.
The relief I felt was incredible, but not as incredible as the feeling of having bub placed on my chest and hearing David introduce me to 'Matilda'. I had such a strong gut feeling throughout my pregnancy that this baby would be a girl, and to hear that my gut feeling was correct made everything fall into place for me immediately. This may sound silly, but not knowing the baby's sex throughout the pregnancy was both exciting and difficult. I wanted so badly to be able to visualise my future child, so I think I had to lean a particular way to help me create this visual. I would have absolutely loved to have had a little boy as well, but to have the vision in my mind match up with reality made things really easy for me. It all just felt meant to be. Hopefully that makes some sense. Basically I just felt so completely elated and nothing else mattered in that moment.
As my placenta was being delivered (I can't put into words the physical relief I felt after this, it was like my preeclampsia symptoms disappeared immediately), Matilda made her way to my breast all on her own, feeding from me within minutes of being born. Her latch was perfect from the get go and the oxytocin high I was riding meant I barely even noticed as I was being stitched back up. Matilda had an Apgar score of 9 at both one and five minutes post birth, so the hospital delivered on its promise of delayed cord clamping and uninterrupted skin to skin time (for both myself and David), only weighing and measuring Matilda once we felt ready for them to.
The next couple of days were a complete blur as Matilda began cluster feeding on day one to bring on my milk quicker, and by day three I was back on my blood pressure medication for postpartum preeclampsia. I was also dealing with a painful episiotomy cut which still to this day feels uncomfortable. All in all, however, I feel I had a positive birth experience. I am so proud of myself for delivering at full term, and for birthing vaginally without an epidural despite being induced. There is nothing more empowering than giving birth and I am so glad and feel so fortunate that I was able to have this experience.
One thing I will mention that did take away from my positive experience was learning after the fact that my hospital was on the list for the "Perineal Protection Bundle". Essentially, the hospital would receive a fine if they allowed a woman to suffer a third or fourth degree tear, and would be awarded money if they performed an episiotomy. Given the 1cm cut they performed on me, I'm guessing a third or fourth degree tear wasn't very likely. If I had known this information prior to giving birth, I never would have agreed to the episiotomy.



Comments